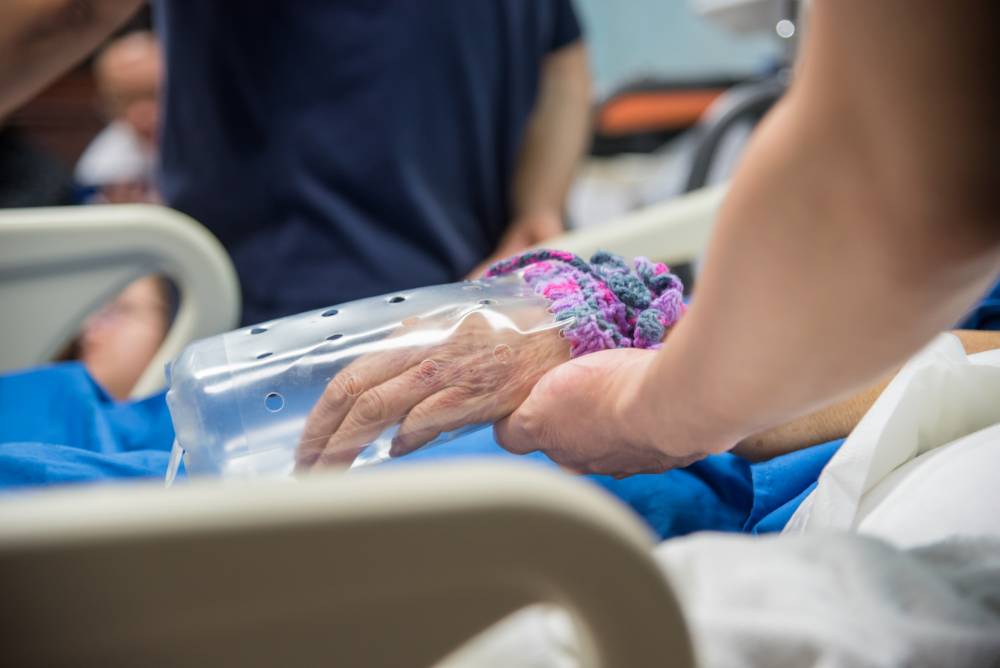
Nearly half of hospital patients diagnosed with dementia were physically restrained to prevent them from harming themselves, according to a new study.
Hospital patients in Japan who are living with dementia were physically restrained to prevent them from trying to get out of bed, trying to pull out catheters, and to prevent the risk of falling, according to the authors of the study.
The study was conducted jointly by the National Cancer Center and the Tokyo Metropolitan Institute of Medical Sciences, and it looked at responses from 937 hospitals across Japan.
The study found that of 23,539 patients with or suspected of having dementia, 10,480 – the equivalent of 45 per cent – were physically restrained during their stay in hospital.
The physical restraints used included tying patients to wheelchairs with belts (28 per cent of the survey cases showed this had been done), enclosing patient’s beds in a barrier (69 per cent), and putting mittens on patients to prevent them from pulling out catheters (26 per cent).
The authors of the study said more research was needed to find better ways to care for the elderly in a country such as Japan, which has a rapidly ageing population – much like Australia’s.
Physical restraints are allowed in hospitals under Japanese law at the discretion of hospital staff.
Physical restraint is permitted in aged care in Australia, but according to the Department of Health’s website, ‘A restraint-free environment is the recommended standard of care.”
According to the Department of Health, the use of physical restraint can cause a deterioration in a resident’s health. It can lead to pain, decreased cognitive function, infection, the development of pressure injuries, falls, and even death.
Yet, the Department says up to half of all aged care residences in Australia use some form of physical restraint.
“Evidence for the prevalence of physical restraint suggests that physical restraint is used in some form for between twelve to forty-nine percent of residents in residential aged care,” the website says.
Family members don’t have the right to ask that residents in aged care be physically restrained, this needs to be determined by the medical practitioner, often in conjunction with a multidisciplinary team.
It’s not hard to imagine how upsetting it would be to be physically restrained. Residents who are restrained probably already feel very unwell, and may be uncomfortable and even angry. To be physically restrained is only likely to make them feel more uncomfortable and distressed.
While the distress caused by restraint is one negative aspect of it, there is also no evidence to suggest that restraint improves a resident’s situation at all.
Evidence actually suggests that physical restraint doesn’t prevent falls, and can actually lead residents to acting on their feelings of frustration.
Dementia consultant Leah Bisiani, in her article ‘Human Rights are not Optional: The Appalling Hypocrisy of Physical Restraint’ says the following:
“Our ethos and duty of care must always support treating others with dignity, kindness, empathy and compassion.
“Use of physical restraints, for any reason bar when critical serious life-threatening danger to a person’s self is indicated, must be considered an inappropriate, horrendously, archaic and barbaric practice, utilized by persons who intentionally traumatize humanity by illegally enforcing abuse.
“It is time to remove the blinkers many people wear when they attempt to justify the brutality behind physical restraint.
“Furthermore, it is an atrocious fact that of all people restraint may be forced upon, people living with dementia pose the highest risk for being restrained when hospitalized.
“Impaired memory, judgment, insight and comprehension; disorientation, a sudden change in environment, acute delirium, pain and distress; all contribute to the difficulty created when a person living with dementia is hospitalized. This is an extremely traumatic experience and often creates fear and terror. The person with dementia may attempt to express this distress by normal responses labelled as unmanageable behavior.
“Older people living with dementia may be defined as high risk to themselves because of their behavioral responses and are thus judged to be ‘unsafe,’ ‘a high falls risk’ or ‘non-compliant to treatment’.
“The miserable reality is that it is often care staff attitudes and mismanagement that create the very behavioral expression and responses that they suggest a person needs restraining for.
“The appalling nature of this treatment has been proven, in majority of cases to be associated with poor outcomes, further functional decline, decreased peripheral circulation, cardiovascular stress, incontinence, muscle atrophy, pressure ulcers, infections, agitation, social isolation, psychiatric morbidity, and serious injuries. The worst scenario being broken bones, strangling, and death; thus creating a horrific situation where someone is placed at increased risk because we do not recognize the repercussions of utilizing physical restraint.
“Physical restraint is a heinous crime and is considered elder abuse.
“I advocate zero tolerance in regard to physical restraint as it defies civilized compassionate care, betrays humanity and disgraces common decency.”
A very good article, very factual, you have obviously worked with people with Dementia. Really enjoyed reading your report.
Thank you Sue for your comment and feedback we are glad you enjoyed it. We do take care when writing and ensure we get the tone right. Have a lovely day.