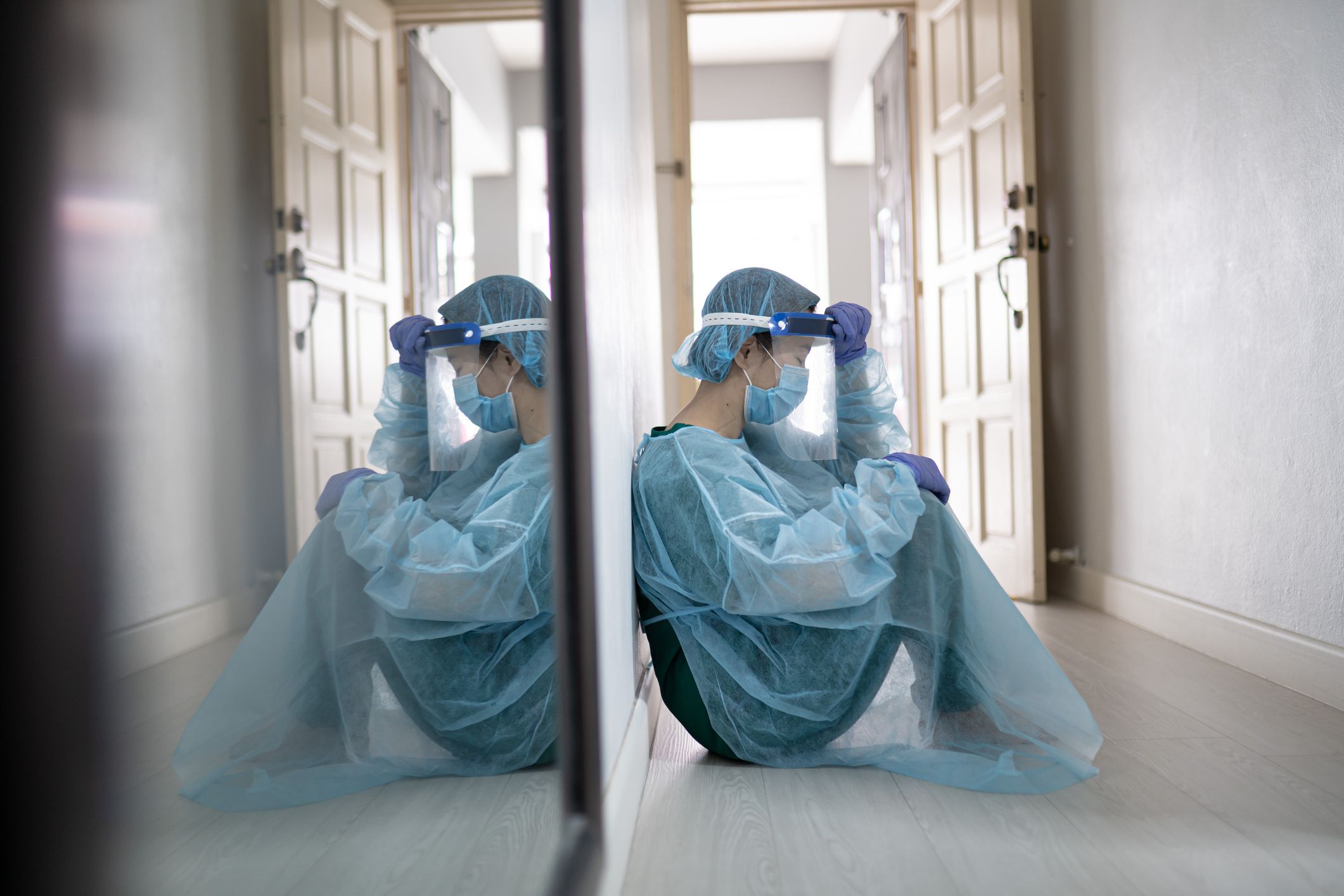
Healthcare workers in New Zealand already face life-and-death decisions daily. But as multiple winter illnesses add pressure to a system already stretched by COVID, staff now also have to deal with daily abuse, acute staff shortages and unsafe working conditions. At times, they cannot provide the care they would like for their patients.
The impact on health workers is often described as stress and burnout. The consequences of this prolonged pressure can be seen in the number of doctors, nurses and other health professionals leaving their jobs for overseas positions and the private sector, or being lost to their professions completely.
Many of these healthcare workers may well be suffering from a more serious form of psychological distress than burnout: moral injury.
Moral injury refers to the psychological, social and spiritual impact of events on a person who holds strong values (such as caring for patients) and operates in high-stakes situations (hospital emergency care), but has to act in a way inconsistent with those values.
Examples include having to turn patients away despite them being in pain or discomfort; being unable to provide adequate care due to staff shortages; and having to care for a dying patient isolated from their loved ones while wearing full protective gear.
Symptoms of moral injury can include strong feelings of guilt and shame (about not being able to uphold healthcare values, for example) as well as high levels of anger and contempt towards the system that prevents proper care.
High levels of self-criticism, loss of trust in people and organisations, and a weakening of personal relationships are further symptoms of moral injury.
It can be viewed as a more severe form of burnout. But while burnout can happen in most workplaces, moral injury requires the three core components listed above.
The term moral injury arose in military psychology to refer to situations where, for example, soldiers were unable to intervene to save lives in case they risked breaching the rules of engagement. More recently, the term has been adapted to apply to healthcare.
Viewing the experiences of health workers through this lens can help us understand why they may experience a seesawing emotional state and the confusing conflict of simultaneously wanting to be at work while wishing they were anywhere but.
For healthcare workers, understanding the concept of moral injury may help reframe it as something that is happening to them rather than because they don’t have the skills to cope. The latter can sometimes be a mistaken implication of the term burnout.
While healthcare workers are largely at the mercy of the organisations they work for, there are some steps individuals can take to alleviate moral injury. Firstly, simply recognising they may be suffering from this condition can reduce confusion and validate their experiences.
Secondly, reconnecting back to an individual’s values and beliefs can help refocus and re-energise, at least temporarily. Reminding themselves why they got into this job in the first place is a useful place to start.
Organisations and businesses must play a lead role in preventing and treating moral injury. Many of the factors leading to it (lack of resources or staff, a pandemic or peak flu season) are outside the control of individuals.
Most modern businesses will be aware they have a legal responsibility under the 2015 Health and Safety at Work Act to look after their employees’ mental and physical well-being.
At a high level, organisations can advocate for systemic change and increases in funding and resourcing, where needed. But these higher-level changes take time to achieve. In the meantime, it is important healthcare workers are protected and supported.
Broad steps an organisation can take to prevent or reduce moral injury include removing the burden of difficult ethical decisions from frontline workers and instead adopting evidence-based policies to guide an organisation-wide response. Where possible, rotating staff between high and low-stress environments may help.
Providing funding for workers to access professional psychological supervision is another practical step businesses can consider. At a team level, it can be helpful to have leaders who are visible, validating and can help make sense of the moral conflict. Leaders can also play a role in keeping alive professional values and modelling their own struggles with the situation.
The general public also has a role to play in supporting healthcare workers. Any steps we can take to protect our own health and thereby reduce pressure on the system can have a cumulative effect on the well-being of doctors, nurses and allied health clinicians. The health of our nation rests with those who work in this field and it is in all our interest that their health is protected and prioritised.
Dougal Sutherland, Clinical Psychologist, Te Herenga Waka — Victoria University of Wellington
This article is republished from The Conversation under a Creative Commons license. Read the original article.