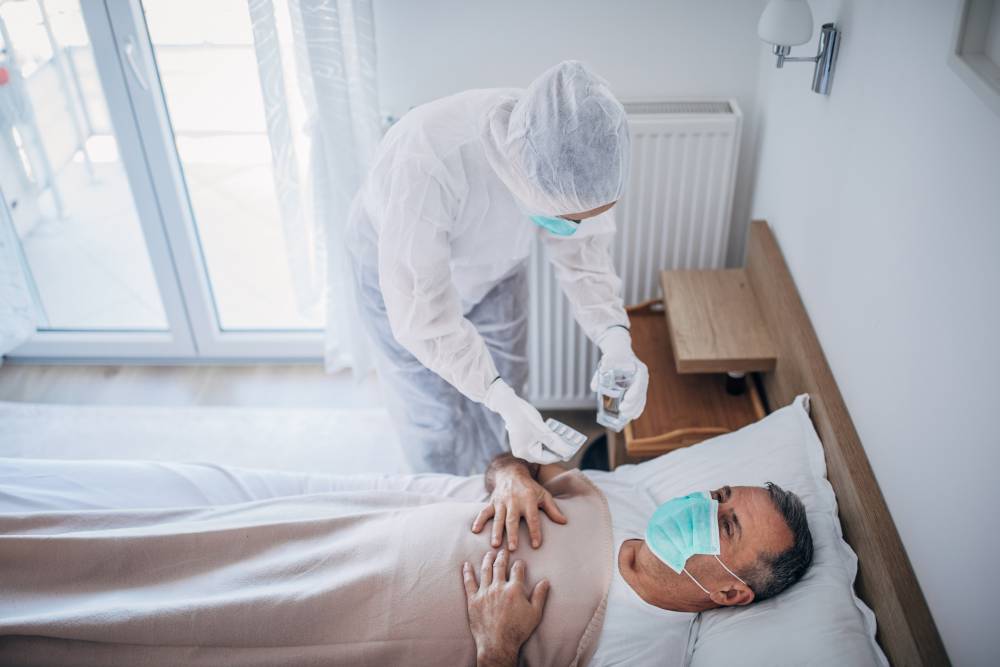
Do staff need to wear Personal Protective Equipment (PPE) when providing aged care services to a suspected COVID-19 case who is awaiting test results?
Aged care workers should wear appropriate PPE when they are providing care to suspected case/s of COVID-19 who are awaiting test results in the interim until their test results are confirmed negative (they do not have COVID-19). The appropriate PPE is known as contact and droplet precautions and requires a gown, surgical mask, eye protection and gloves.
If the suspected COVID-19 case is confirmed positive and staff who were in close contact with the client did not use appropriate PPE, these staff will be required to notify their employer and self-quarantine for 14 days.
If the suspected COVID-19 case is confirmed positive and staff who were in close contact with the client did use appropriate PPE, these staff can continue to provide care to the client, and other clients, and do not need to self-quarantine.
What is close contact?
Close contact is defined as meeting the following criteria:
Do staff need to wear PPE when providing aged care services to a close contact of a confirmed COVID-19 case (and the close contact is in quarantine for 14 days)?
Aged care workers do not need to wear any additional PPE, above appropriate contact precautions where required, if they have only been exposed to a close contact who does not have symptoms of COVID-19.
Aged care workers only need to wear additional PPE, known as droplet precautions (including gown, surgical mask, eye protection and gloves) when providing care to a close contact of a COVID-19 case when:
Do staff need to wear PPE when providing aged care services when there is a confirmed COVID-19 case in the facility they work in but they have not had any contact with this case?
Aged care workers do not need to wear PPE when providing aged care services if they have had no close contact with a confirmed COVID-19 case in their facility.
Additional guidelines on the use of PPE when caring for patients in the non-inpatient setting are available on the department’s website.
If you have any questions about the use of PPE or if you require PPE, email agedcarecovidppe@health.gov.au
Hi just a question when a resident has come from hospital and is isolated for 14days .. as a precaution should care staff wear PPE in this situation… these residents are confined to one section of the nursing home I am and so are the rest of co workers concerned cos I do have family that I don’t want to pass any Coronavirus to
How do you know beforehand that the person you’re in close contact with is going to start showing symptoms in 24 hours time? When the people I’m caring for start showing symptoms, how do I go back in time and wear a mask for the previous 24 hours?
This is true for any virus they may have & if you are being cautious you should be fine as this is droplet precautions, not airborne. Wear gloves when likely to come in contact with bodily fluids, wear your eye protection (all nurses should have their own goggles that they carry with them every shift) & adhere to your universal precautions…above all, don’t panic.
Do have to wear face mask when visiting Age care home