
New research confirms what most of us may have intuitively already known – that nurses are able to accurately predict a patient’s decline, and are therefore a vital source of information when it comes to saving lives.
The research by the Mayo Clinic in the United States looked at how accurately a patient’s decline is detected – identifying a decline early is vital in preventing further deterioration or even death.
For example, sepsis and acute respiratory failure have a mortality rate of 20-30 per cent in the US, and are involved in 34-52 per cent of hospital deaths. Mortality rates are higher if intervention is delayed, according to the researchers.
One way to detect a deterioration in a patient’s health is to use an automated scoring system based on data from electronic health records. Results to date from these systems have not been encouraging – the electronic records are not accurately able to predict declines.
“Early warning scores do not demonstrate accurate predictive capabilities when applied strictly, and to date they have failed to provide strong evidence of their ability to improve outcomes,” the research paper states.
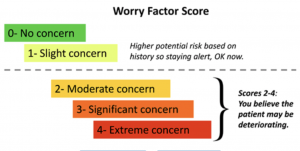
The study looked at a measure of a nurse’s worry about the patient’s condition, called, appropriately, the “worried criterion”. The measure is based on a nurse’s pattern recognition, and is based on a five-point scale: 0 for no concern the patient is deteriorating to 4 for extreme concern the patient is deteriorating.
The study involved 3,185 patients during 3,551 hospitalisations.
The study found that nurses were able to predict a decline in 77 per cent of cases. Nurses with more experience had higher rates of accuracy.
A patient with a ‘worry factor’ of 3 or more was 40 times more likely to require transfer to an intensive care unit within the next 24 hours.
“The nursing staff’s sense of worry, whether through analytical skills or through pattern recognition, is very accurate in identifying deteriorating patients and should be more consistently valued and utilized, considering incorporation into the medical record,” the researchers wrote.
Detecting a patient’s decline is clearly vitally important because it is the best way to avoid deterioration.
The research shows that objective measures, such as neurological, skin or nutritional status, are not as accurate in making predictions about the patient’s risk of deterioration as a nurse’s more subjective assessment.
Austrlian Nursing and Midwifery Federation Federal Secretary, Annie Butler, told HelloCare, nurse’s expertise is widely acknowledged.
“The importance of nurses’ expert clinical judgement for timely recognition and response to clinical deterioration (including pattern recognition and intuitive ways of knowing) has been known for a long time,” she said.
Previous studies have concluded that: “The value of ward nurses’ ability to recognize and respond to patient’s deterioration, reduce adverse events and promote patient safety cannot be understated,” Ms Butler said.
“Doctors have also known this for a long time,” she added. “Many doctors have told us how important it is to listen to nurses – if the nurse is worried, then usually, they need to be worried.”
In regards to recognising patterns and changes for patients, Ms Butler said nurses acquire this skill through training, experience and their close contact with patients and, in aged care, residents.
“Nurse acquire their skills through formal education, training, and clinical placements; they then develop these skills through practising, utilising evidence, knowledge and research, as well as through processes of professional socialisation where they learn from experienced nurses, and other clinicians, how to develop a comprehensive and holistic picture of patients in their care.
“Nurses’ are the health professionals positioned most closely to the patient; they spend the most time with the patient and are frequently the health professional who is involved in the most intimate activities with patients.
“Nurses can often recognise change in a patient before the change is reflected in clinical evidence of the decline”, Ms Butler said.
“This constant engagement coupled with their scientific knowledge and understanding and holistic philosophy, means that nurses not only understand when a change in a patient’s condition is significant but also sees them ideally placed to identify changes even before technical assessments and ‘machines’ identify a change,” she told HelloCare.
While the research relates to a hospital setting, Ms Butler said the findings “without question” are just as applicable in aged care. However all too often nurses are not able to apply their judgement because they are either not on site, or unable to spend enough time with residents due to low staff numbers.
“As is becoming increasingly evident through the stories unfolding in the Royal Commission, the current environment in aged care is not allowing nurses’ clinical judgement and intuition to be used to its full capacity.
“Too often, a nurse is not available on site in aged care settings, or they are only available by phone, which inhibits the nurse’s ability to assess and observe what’s happening with the resident or elderly person,” Ms Butler said.
“Often, even when they are on site, the current ratios in many aged care settings, eg 1 RN to 60/80/100 residents simply does not give nurses the time needed to develop the understanding needed to inform expert clinical judgement and decision-making.”
Ms Butler said she would like to “better acknowledgment” of nurses’ skills as well as better resourcing so nurses are able to use the full breadth of their skills.
The necessary resources are “often available in large tertiary acute care facilities, particularly where there are mandated minimum staffing levels, such as Victoria and Queensland,” Ms Butlers said.
“Support also involves adequate medical staff, who can be available to respond and act quickly on nurses’ concerns.”
“The aged care setting is poorly lacking in the level of support required to ensure that nurses are able to practise to their full capacity, both in terms of adequate nurse staffing and access to medical support,” Ms Butler said.
“This lack of support is a major contributor to the levels of missed care we are seeing in the aged care sector and many of the poor care outcomes.
“It is yet another reason why mandated minimum staffing levels and appropriate skills mix are so urgently needed in aged care,” she concluded.
This is so very true! Unfortunately new nurses are taught to rely on scoring on computer assessments to determine a patient’s status and not to consider intuition. Certainly not all nurses are intuitive, but many of the older ones are. I often could not pinpoint what prompted my concern for a resident when all their vital signs were good, but I just knew, and I was rarely wrong.
Absolutely true. I have been retired for twenty years after forty three years in active nursing and still retain that intuitive ability with people I know well in the family and church I attend. In my Gerontic studies we were taught that changes can occur in an elderly person even six months prior to their eventual death. With my own mother I told the nursing staff that this change was apparent a month before she passed away and the response was that she was fine. It is something a nurse develops over time and sometimes isn’t conscious of .